Understanding Advanced Directives (Healthcare)
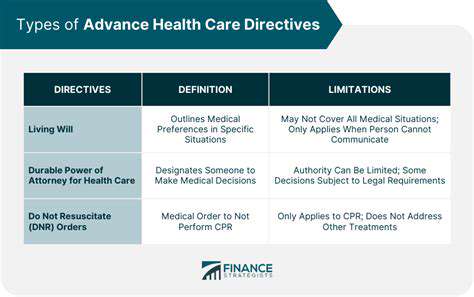
Types of Advanced Directives
Living Wills
Living wills are legal documents that outline a person's wishes regarding medical treatment if they become incapacitated and unable to communicate their desires. These documents typically specify the types of medical interventions a person wants or doesn't want, such as life-sustaining treatments like mechanical ventilation or feeding tubes. Living wills are crucial for ensuring that medical decisions align with the individual's values and preferences, providing guidance for healthcare providers and loved ones during challenging times. They play a vital role in respecting patient autonomy and ensuring that treatment choices reflect the patient's current wishes, not just their past opinions.
It's important to remember that living wills are not a substitute for ongoing communication with healthcare providers and loved ones. Regular discussions about preferences and values are essential to ensure that the living will accurately reflects the individual's current intentions. A living will should be reviewed periodically to ensure its continued relevance and to make necessary updates to reflect any changes in the individual's wishes or circumstances.
Durable Power of Attorney for Healthcare (DPAHC)
A Durable Power of Attorney for Healthcare (DPAHC) designates a trusted individual to make healthcare decisions on behalf of the principal if they lose the ability to do so. This agent, or healthcare proxy, is empowered to make decisions consistent with the principal's wishes, as documented in the DPAHC or through conversations with the principal. This document is vital for ensuring that someone understands and carries out the patient's wishes when they are unable to do so themselves. It's crucial to choose a proxy who is reliable, trustworthy, and has a good understanding of the patient's values and preferences.
The DPAHC differs from a living will in that it appoints a person to make decisions, whereas a living will directly outlines specific medical treatments. Ideally, both documents work together to provide a comprehensive approach to ensuring a patient's wishes are respected in the event of incapacity.
Healthcare Proxies
Healthcare proxies, often referred to as health care agents, are individuals appointed to make medical decisions on behalf of another person. These individuals are chosen by the patient and should be someone who understands and respects their values and preferences. Healthcare proxies step into the decision-making role when the patient is unable to communicate their choices. They have the authority to make decisions about various aspects of healthcare, from treatment choices to end-of-life care, ensuring that patient autonomy is preserved even when the patient is incapacitated.
The selection of a healthcare proxy is a critical step in ensuring that a patient's wishes are honored. Open communication about values and preferences is important to build trust and ensure that the appointed proxy understands the patient's priorities. The appointment of a healthcare proxy is a crucial aspect of advanced directives, providing a mechanism for maintaining patient autonomy and control over medical decisions.
Do Not Resuscitate (DNR) Orders
Do Not Resuscitate (DNR) orders are legal documents that instruct medical professionals not to perform cardiopulmonary resuscitation (CPR) in the event of cardiac or respiratory arrest. These orders reflect a patient's desire to avoid aggressive life-sustaining measures and are an important component of end-of-life care planning. DNR orders provide clarity and guidance to healthcare providers, allowing them to respect the patient's wishes for a natural death. They are crucial for ensuring that treatment decisions align with the patient's values and preferences, promoting a peaceful and respectful end-of-life experience.
Advance Care Planning
Advance care planning is the overarching process of considering and documenting future healthcare preferences, including the creation of advanced directives like living wills and DPAHCs. It's a proactive way to ensure that medical decisions align with a person's values and preferences, even when they are unable to communicate them directly. This process involves open communication with loved ones, healthcare providers, and the development of clear documents that outline treatment choices. Advance care planning empowers individuals to take control of their healthcare decisions and ensures that their wishes are known and respected in the future.
Engaging in advance care planning is vital for individuals of all ages and health statuses. It's a thoughtful and proactive way to ensure that healthcare decisions are made in accordance with personal values and preferences, promoting peace of mind and facilitating compassionate end-of-life care.

Accessing Legal and Medical Assistance
Understanding Your Rights and Responsibilities
Navigating the complexities of healthcare decisions can be daunting. Knowing your rights and responsibilities as a patient is crucial when considering advanced directives. This involves understanding the legal frameworks surrounding healthcare choices, including the capacity to make those choices and the potential limitations on medical intervention. Comprehending these rights empowers you to make informed decisions that align with your values and preferences.
Choosing a Healthcare Proxy
A healthcare proxy, often referred to as a durable power of attorney for healthcare, is a vital component of advanced directives. This designated individual is empowered to make medical decisions on your behalf if you lose the capacity to do so. Careful consideration should be given to selecting someone you trust implicitly, who understands your values, and who is comfortable acting as your advocate in sensitive healthcare situations. This appointment is a critical step towards ensuring your wishes are honored.
It's important to discuss your wishes with your chosen proxy and ensure they are comfortable with this role and understand the implications involved. This open communication will help avoid misunderstandings and ensure your wishes are carried out effectively.
Creating a Living Will
A living will is a legal document that outlines your preferences regarding medical treatment if you become terminally ill or incapacitated. This document often addresses specific interventions like life-support, resuscitation, and pain management. Having a living will helps ensure that your healthcare team understands your wishes and allows them to act accordingly, respecting your autonomy regarding life-sustaining measures.
Understanding Advance Care Planning
Advance care planning encompasses the entire process of discussing, documenting, and communicating your healthcare preferences. It's more than just creating documents; it's about having open conversations with loved ones and healthcare professionals. This proactive approach empowers you to maintain control over your medical future while providing clarity and support to those around you.
Regularly reviewing and updating your advance directives is an essential part of advance care planning. Life circumstances can change, and your preferences might evolve over time. Ensuring your documents reflect your current wishes is crucial for maintaining your autonomy and ensuring your healthcare team understands your decisions.
Legal Implications of Advanced Directives
Understanding the legal implications of advanced directives is essential to ensure their validity and enforceability. Different jurisdictions may have specific requirements for the format and execution of these documents. It's crucial to consult with legal professionals to ensure your documents comply with all applicable laws and regulations. This legal expertise ensures the documents are legally sound, safeguarding your wishes and preventing potential conflicts.
Medical Assistance for Decision-Making
Seeking medical assistance in the process of creating and understanding advanced directives is crucial for ensuring your decisions are well-informed and aligned with your health status. Your physician can offer valuable insights into medical conditions and treatment options, helping you make informed choices that align with your values. Medical professionals can also provide guidance on the legal implications of your decisions and help you ensure all documentation is accurate and complete.
Read more about Understanding Advanced Directives (Healthcare)
Hot Recommendations
- Tax Planning Tips for Homeowners [2025]
- How to Get Insurance for a Short Term Rental Property
- Understanding the Benefits of a Roth IRA
- How to Manage Business Debt After a Downturn
- How to Use a Barbell Investment Strategy
- Best Ways to Track Your Progress Towards Financial Freedom
- Tips for Managing Credit Card Rewards While Paying Off Balances
- Tax Planning Tips for Stock Options
- How to Plan for Retirement if You Didn't Save Early
- Guide to Managing Legal Debt